The Polio Vaccine
The polio vaccine provides lifelong immunity and is the only means of polio prevention. There are two types currently available: the oral polio vaccine (OPV) and the inactivated polio vaccine (IPV). The vaccine results in humoral (circulating antibody) and mucosal
(circulating antibody) and mucosal (secretory immunoglobulin A) immune responses (27).
(secretory immunoglobulin A) immune responses (27).
Oral Polio Vaccine (OPV)
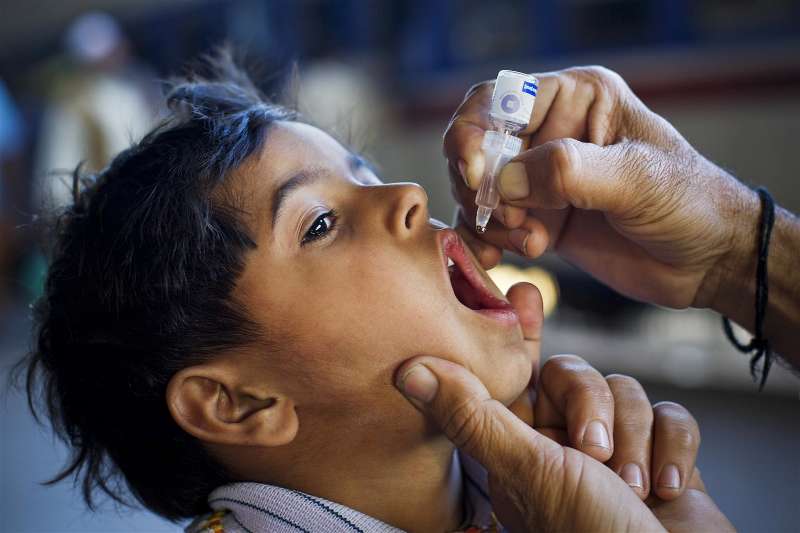
Figure 18 Oral Polio Vaccine being administered to a child (28)
Albert Sabin's OPV is a live vaccine. It is much less expensive than the injectable vaccine and is easy to administer by mouth. OPV provides short-term intestinal immunity to wild polioviruses and long-term humoral immunity against paralytic polio disease (29). OPV given at or soon after birth increases antibody levels and seroconversion rates of subsequent doses (27).
rates of subsequent doses (27).
However, while rare, OPV can cause paralytic polio and those who are vaccinated using OPV, as well as their unimmunized contacts, are at risk of developing paralytic polio. The risk is estimated to be 4 cases per 1,000,000 births annually in countries administering OPV, a slim risk though possible (27).
Inactivated Polio Vaccine (IPV)
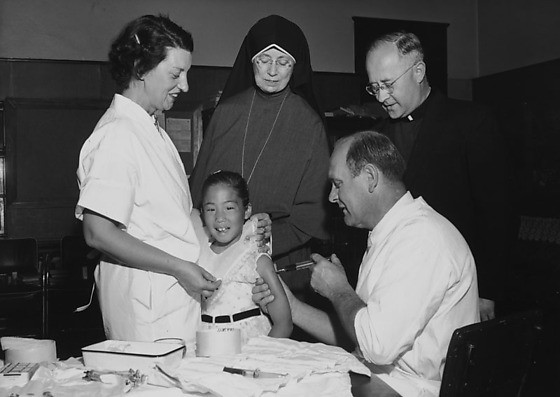
Figure 19 Children given polio vaccine at Maryknoll School, Los Angeles, California, May 19, 1955 (30)
The IPV, created by Dr. Jonas Salk, is administered by intramuscular or subcutaneous injection. IPV is one of the safest routine vaccines, but it is more expensive and more difficult to administer than OPV. IPV also triggers a lower level of immunity in the intestine than OPV (31).
As polio rates decrease or are eliminated, many countries have added or switched to sole use of IPV due to the risks associated with OPV (29). Once all wild poliovirus is eradicated globally, only IPV will be used (29).
Vaccine-Derived Polio
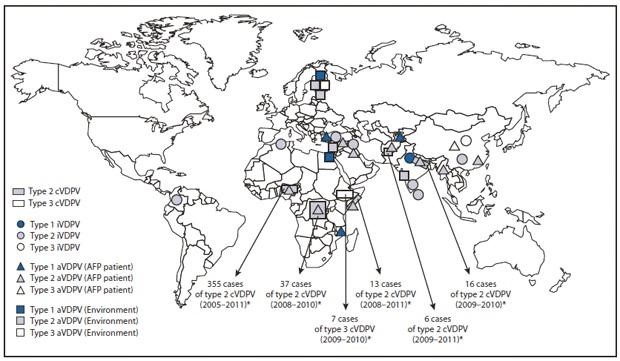
Figure 20 Vaccine-derived polioviruses (VDPVs) detected worldwide, July 2009 - March 2011 (29)
| Map Key:
cVDPV = circulating VDPV iVDPV = immunodeficiency-associated VDPV aVDPV = ambiguous VDPV AFP = acute flaccid paralysis |
Because receipt of the oral polio vaccine results in the shedding of the weakened vaccine-virus in feces, in areas of poor sanitation with populations that are under-immunized, if an excreted vaccine-virus is allowed to circulate for at least one year, it can mutate into circulating vaccine-derived poliovirus (cVDPV), which causes paralysis. 20 outbreaks of cVDPV have been recorded in 20 countries to date (32).
In rare cases, individuals with primary immunodeficiencies have been administered the oral polio vaccine prior to diagnosis of immunodeficiency, and contracted vaccine-derived poliovirus. Studies indicate that they have then shed polio in their stool for up to several years (15). Notably, HIV/AIDS does not seem to be a risk factor of those with immunodeficiencies experiencing this effect (27).
